Rheumatoid Arthritis: Understanding the Disease and Biologic Treatment Options
 Mar, 31 2026
Mar, 31 2026
Rheumatoid Arthritis isn't just regular joint ache.
It is a complex condition where your own immune system accidentally targets healthy tissue.
If you wake up gripping your hands tight because they won't open, or feel a deep burn in your knees after sitting still, you know this pain differs from typical wear-and-tear. Many people mistake early signs for aging, but the pattern of swelling tells a different story. By understanding what is happening inside your joints, you take the first step toward managing the discomfort effectively.
What Really Happens in Your Joints?
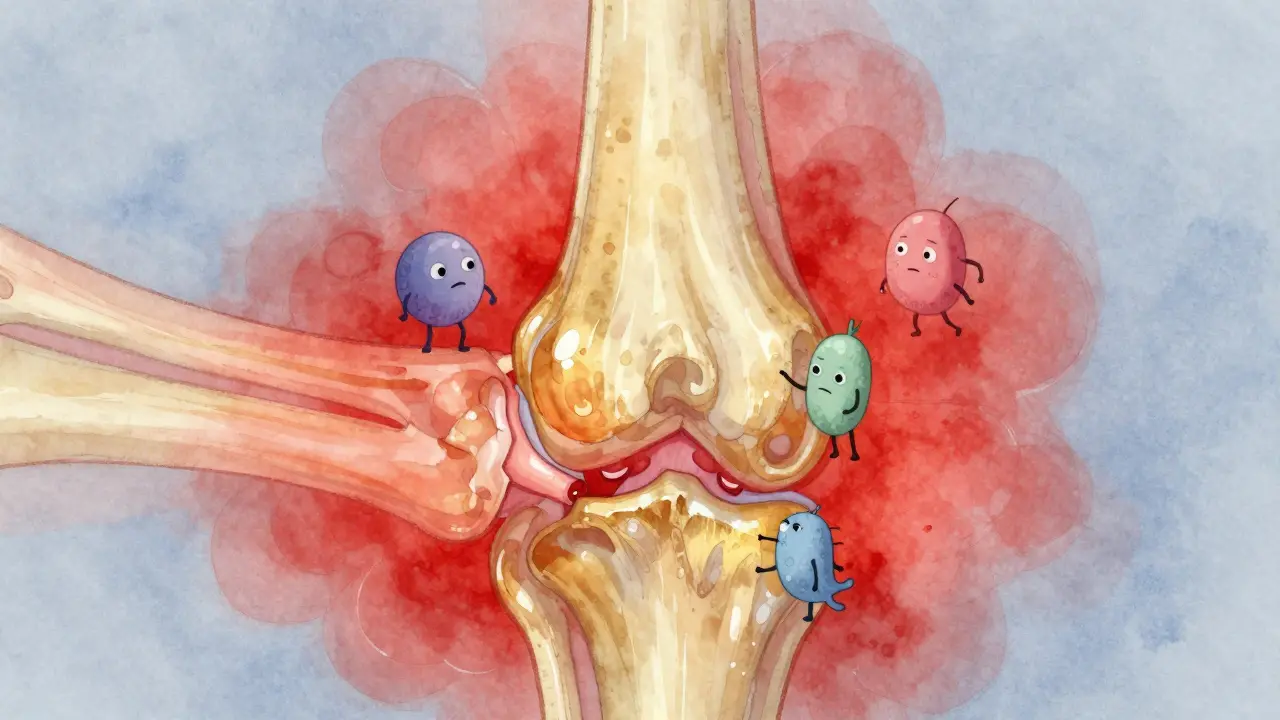
To understand why biologics work, we have to look at the machinery of inflammation. Normally, your body fights bacteria and viruses. With Rheumatoid Arthritis, that defense system turns inward. It targets the synovium, which is the thin lining covering most of your joints. When this lining gets inflamed, it thickens and produces too much fluid. This pressure eventually erodes the cartilage between bones and creates damage that doesn't heal easily.
Autoimmune diseases occur when the immune system attacks the body's own healthy tissues. This specific malfunction distinguishes the condition from osteoarthritis, which is mechanical wear-and-tear. While osteoarthritis hurts more after activity, rheumatoid arthritis often stiffens you up in the morning. That morning stiffness, lasting more than 30 or 45 minutes, acts as a major red flag doctors watch for.
Detecting the Early Signs
Catching the disease early saves your joints. Most experts agree that starting aggressive treatment within the first few months stops permanent damage. You won't always see a lump right away. Instead, look for symmetrical symptoms-if your left wrist hurts, your right wrist likely does too. Doctors rely on specific markers to confirm what you feel. They look for antibodies in your blood, such as rheumatoid factor (RF) or anti-cyclic citrullinated peptide (anti-CCP). Even if these tests come back negative, a doctor might still diagnose the condition based on how your joints behave.
Imaging also plays a huge role. X-rays show bone changes, but ultrasound or MRI scans reveal inflammation earlier, showing fluid in the
The Role of Traditional Medication
Before trying advanced therapies, doctors typically prescribe a foundational medication. Methotrexate is widely considered the gold standard for initial care. It works by slowing down the immune system generally. For many, this oral pill reduces inflammation enough to stop the disease progress without needing injections. However, not everyone responds well enough to it alone, and some find the side effects difficult to manage.
Disease-modifying antirheumatic drugs (DMARDs) aim to alter the course of the disease process. These traditional drugs help, but they lack precision. Imagine throwing a net over a pond to catch fish; sometimes you catch what you want, sometimes you catch debris too. Biologics offer a different approach entirely.
How Biologic Therapies Work
When traditional options aren't enough, biologics provide a laser-focused solution. These medications target specific proteins driving the inflammation rather than dampening your entire immune response. They are protein-based molecules manufactured in living cells. Because they interact with precise parts of the biology, they fit under the category of targeted synthetic treatment.
| Drug Class | Target | Common Examples | Administration |
|---|---|---|---|
| TNF Inhibitors | Tumor Necrosis Factor | Adalimumab, Etanercept | Injection |
| IL-6 Inhibitors | Interleukin-6 | Tocilizumab | IV Infusion or Injection |
| B-Cell Targeting | B-Lymphocytes | Rituximab | IV Infusion |
| JAK Inhibitors | Intracellular Pathways | Upadacitinib | Pill |
The most famous group involves TNF Inhibitors. These block a specific substance called Tumor Necrosis Factor-alpha, which fuels the inflammatory fire in your joints. Drugs like Humira (adalimumab) fall here. They can reduce active inflammation significantly, helping you regain movement in fingers that were previously stuck. Another option focuses on interleukin-6 (IL-6), a messenger chemical that signals cells to make more inflammation. Blocking this pathway helps patients who didn't respond to TNF inhibitors.
Some newer options target B-cells or T-cells directly. These adjust the number of white blood cells responsible for the attack. Because each person's immune biology varies slightly, what works for one patient might not help another. This is why finding the right fit often requires patience and close monitoring by a Rheumatologist.
Weighing Benefits Against Risks
While biologics offer hope for remission, they aren't without trade-offs. The biggest concern is infection. Because these drugs suppress specific immune pathways, they can lower your body's defenses against germs. Data shows patients face a slightly higher risk of serious infections compared to those on standard meds. Simple precautions like getting flu shots or avoiding crowds during high-risk seasons become essential habits.
Cost is another major factor. Without insurance assistance, these treatments are expensive. Annual costs often reach into tens of thousands of dollars. However, manufacturer support programs have improved recently to help offset these burdens. Additionally, the emergence of biosimilars-high-quality generics for biologics-is starting to lower prices. As of early 2026, new approvals for biosimilar versions are making access easier for budget-conscious patients.
Long-term safety monitoring remains standard. Doctors run blood tests regularly to check liver function and blood counts. They also screen for tuberculosis before starting treatment, as suppressing immunity can reactivate dormant TB bacteria. Despite these hurdles, studies indicate that achieving low disease activity through biologics improves quality of life metrics significantly compared to uncontrolled disease states.

Managing Daily Life with the Condition
Medication handles the chemistry, but your daily choices influence the outcome too. Staying active keeps joints moving and maintains muscle strength. Physical therapy exercises help counteract the stiffness that comes with inactivity. Losing even 5% of your body weight can decrease stress on load-bearing joints, reducing pain levels naturally.
Mental health matters just as much as physical health. Chronic pain leads to anxiety or depression in many cases. Connecting with support groups, either locally or online, provides practical advice and emotional reassurance. Remember that flare-ups happen, but consistent management keeps them manageable. If one medication stops working, switching strategies is common, not a failure.
Can Rheumatoid Arthritis ever be cured?
Currently, there is no permanent cure. However, modern treatment goals aim for clinical remission, where symptoms disappear and joint damage stops progressing. Many patients live symptom-free for long periods with proper therapy.
Are biologics safe to take long-term?
Most patients tolerate them well. Safety monitoring is required due to risks of infection and rare complications like lymphoma. Regular check-ups and vaccinations keep these risks low.
When should I ask for biologic therapy?
If you have been on Methotrexate for at least 3-6 months and still have high disease activity, discuss adding or switching to a biologic agent with your specialist.
Do these drugs cause weight gain?
Biologics themselves rarely cause direct weight gain, but increased appetite from feeling better might lead to eating more. Steroids prescribed alongside can definitely increase weight.
Is there a genetic link to this condition?
Yes, genetics play a role. Certain gene variations increase susceptibility, but environmental triggers usually start the actual disease process.
Looking Ahead
The landscape for treatment evolves constantly. Researchers are currently testing biomarkers that predict which drug will work best for a specific individual profile. Future approaches may involve stopping treatment once stability is reached, sparing patients years of unnecessary medication exposure. For now, the combination of early detection, targeted drugs, and proactive lifestyle management gives you the strongest control possible.
If you suspect you have symptoms, do not wait. Every month of delay allows more potential structural damage. A proper evaluation sets the stage for a strategy that preserves your mobility and independence.

Russel Sarong
April 2, 2026 AT 08:51The pain! It feels like fire rushing through your veins when you wake up!!! You grip your hands because the joints simply lock up completely!!! The swelling pattern tells a story nobody wants to hear!!!!! If you ignore the morning stiffness for weeks your bones start eating themselves alive!!!!! This is not normal aging! This is an immune system betrayal!!!!!
Sharon Munger
April 4, 2026 AT 07:32Methotrexate remains the foundation for most treatment plans today. Many patients find relief within six months of starting therapy. Symmetrical symptoms are the key indicator for diagnosis. Insurance coverage varies significantly by region and provider.
Julian Soro
April 5, 2026 AT 05:54Early intervention really does save the joint function long term. Starting biologics sooner prevents irreversible erosion. Physical therapy helps maintain range of motion while meds handle inflammation. Support groups provide essential coping strategies for daily stress.
Christopher Beeson
April 6, 2026 AT 23:31The cost barrier is absurd for these targeted therapies. Why must healthcare tie survival to employment status? The pharmaceutical lobby ensures prices stay artificially high. We wait years for biosimilars to trickle down to the masses. Patient safety takes second place to profit margins always.
Rod Farren
April 8, 2026 AT 15:24Tumor Necrosis Factor-alpha inhibitors disrupt the cytokine cascade effectively. Interleukin-6 blockade provides alternative signaling pathway suppression. B-cell depletion reduces autoantibody production rates significantly. JAK inhibition offers oral convenience with intracellular kinase targeting specificity.
Jenny Gardner
April 8, 2026 AT 20:56The distinction between osteoarthritis and rheumatoid arthritis is clinically vital for prognosis!! Diagnostic imaging modalities have evolved considerably over the past decade!!!!! MRI scans detect synovitis before bone erosion becomes visible on plain films!!!!! Accurate testing protocols include anti-CCP antibodies and RF titers!!!!!
Cullen Zelenka
April 10, 2026 AT 06:40Seeing people describe the morning stiffness really resonates with my experience too. It is great that we have better options now than just managing the pain. Staying positive about remission goals keeps hope alive for everyone. Movement really does help counteract the stiffness naturally.
Owen Barnes
April 10, 2026 AT 15:31I think the jargon regarding the kinase inhibitors is importent for understanding the mechaism of action. People shoudl talk to their rheumatalogist about which pathway is best for thier bioligies. Cost assistence programs exist to help pay for the meseines. It is good to know the science behind the treatments.
Eleanor Black
April 10, 2026 AT 17:51It is truly remarkable how far medical science has progressed in managing autoimmune conditions like this.
Many individuals feel overwhelmed by the complexity of the different drug classes available today.
Understanding the difference between traditional DMARDs and newer biologics is incredibly important for patient empowerment.
Insurance barriers remain a significant hurdle for those needing advanced therapeutic interventions regularly.
We must continue to advocate for broader access to these life-changing medications globally.
Patient education plays a massive role in achieving long-term clinical remission successfully.
Daily habits such as maintaining a healthy weight reduce physical stress on inflamed joints significantly.
Support systems provide emotional stability during periods of disease flare-ups or adjustment.
Monitoring infection risks requires consistent vigilance alongside standard blood work screenings.
Vaccination schedules should be updated proactively to prevent opportunistic infections during treatment.
Regular communication with specialists ensures medication efficacy is optimized over time.
Research continues to refine predictive biomarkers for personalized treatment selection strategies.
Hope remains abundant despite the chronic nature of this challenging health condition overall.
Every step taken toward early detection preserves future quality of life substantially.
Together we face this journey with courage and informed medical partnership always.
Callie Bartley
April 12, 2026 AT 13:41Focusing entirely on profit while patients struggle creates unnecessary suffering everywhere. It seems obvious that accessibility is ignored for shareholder returns repeatedly. One would expect more compassion in these critical healthcare discussions today.
Molly O'Donnell
April 13, 2026 AT 21:10Clinical correlation is required alongside imaging results for accurate diagnosis.
Arun Kumar
April 14, 2026 AT 05:01Thank you for sharing such detailed information on diagnostic imaging and testing markers. Learning about the specific antibodies helps us understand the body better. Keep sharing your insights as we navigate these health topics together.